Blood Type and the Microbiome |
More and more, we hear and read about the importance of the microbiome, the ecological community of friendly and unfriendly microorganisms that share our body space. The human body contains as much as ten times more microbial organisms than human cells, and increasingly, changes to the microbiome are being associated with alterations, both good and bad, to our health. Blood Type Connections Most laypeople and physicians can be forgiven for wondering what could blood type possibly have to do with the microorganisms in the digestive system. Blood type, after all, is just an ornament on a red blood cell, right? A complication of transfusion. Sadly, not much else about blood type is taught as part of the standard medical curriculum. However readers of my books and followers of my diet theory already know that there is a much deeper and important role that blood type plays in conditioning our digestive tract; both in terms of the characteristics of the lining (mucosa) and the variations of the secretions (digestive juices) produced by the stomach and intestines. These blood type specific differences can themselves have an important effect in altering the microbial balance of the digestive tract. But there are even more elemental and direct ways that blood type can condition the microbiome. The blood type antigens (the marker that distinguishes one ABO blood type from another) are widely distributed throughout the digestive tract, embedded in the mucus lining that insulates the gut tissue from the rather harsh internal environment. The most common blood group antigens are proteins that contain the sugar fucose. This the most basic building block, and is called the H antigen. Although we commonly think of blood type O and not possessing a blood group antigen: The name 'O' was chosen to signify the number zero. The rationale behind that label only relates to the fact that type O blood does not trigger an immunologic reaction when transfused into the other ABO types. Type O blood does in fact possess an antigen, the so-called 'H' antigen. However since all the other ABO types also make H antigen, it is not immunologically reactive in them, and allows type O to function as the 'universal donor.' So, to tie this important relationship together, let's put it in a table: Blood Type Antigens as Bacterial Snack Food There is good evidence that the ABO blood type antigens are a major influence on the specificity of the bacterial enzymes produced the microbiome, serving to 'condition' the microbiome. Much like how putting sunflower seeds into your bird feeder will tend to encourage Cardinals to hang out in your backyard, the microbiome of a person who is blood type B will tend to have bacteria with a preference and enzyme capacity for degrading the B-antigen. Human feces contain enzymes produced by the bacteria of the microbiome that degrade (break down and metabolize) the A, B and H blood type antigens lining the digestive tract and convert it to an energy source for their own use. The population of fecal bacteria that produce blood group-degrading enzymes is highly correlated with the ABO and secretor type of the host. In fact, blood group specificity is common among intestinal bacteria with almost 50% of strains tested showing some blood type A, B, or O specificity. To give you an idea of the magnitude of the blood type influence on intestinal microflora, it has been estimated that someone with blood type B will have up to 50,000 times more of some strains of friendly bacteria than either blood type A or O individuals. Thus you might be surprised to discover than much of a healthy microbiome is the result of harboring bacteria that like to 'Eat Right for Their Blood Type.' 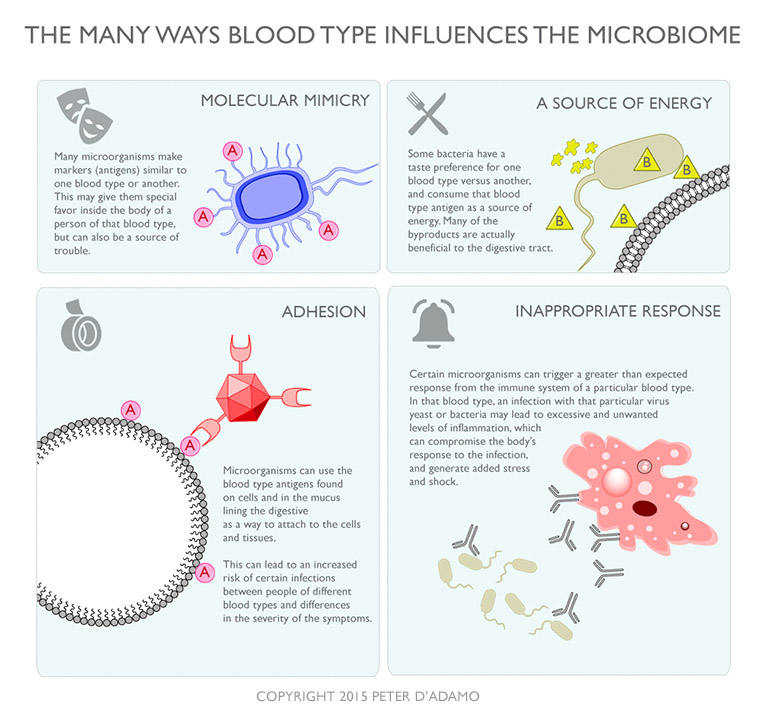
Blood Type Antibodies as Nightclub Bouncers Although the average physician does not consider blood type antibodies beyond their role as a transfusion nuisance, common sense dictates that they serve a more basic role; natural selection obviously can not predict this type of need, despite its obviously life-saving benefits. Instead these antibodies work in combination with the antigens to create a molecular and immunologic 'line in the sand,' allowing microbial species with similarity to the antigen to avoid immune reaction, while targeting dissimilar strains for destruction. A large percentage of microogranisms share antigenic similarity with the ABO blood type antigens, which in themselves are nothing unique or special to humans. Thus, if you are a critter who has developed a similar antigen to the blood type antigen, you'll probably do fairly well in the gut of blood type A humans. On the other hand you are probably going to have real difficulties should you find yourself inside the body of a type B, as they carry antibodies (extremely powerful ones, by the way) to type A and will not like you very much at all. Many studies have associated increases in the blood type antibodies during many common infections, and the ability of type O to manufacture both anti-A and anti-B antibodies may have given them a real advantage when it came to natural resistance to many pathogenic bacteria and viruses. However similarity between your blood type antigen and the antigens on a microbe are no guarantee of future harmony. Just like an uninvited guest can sometimes get past the nightclub bouncer by claiming that 'I'm with the band,' microbes with ill-intent can evade the basic defenses by developing the ability to mimic the blood type antigen of their potential host/victim. Just as in Star Trek, this 'cloaking device' gives them a degree of invisibility from the immune system. In one study, microbial antigens crossreacting with blood group antigens were detected on cell walls of anaerobic bacteria from three of 10 cultures inoculated. (17) Other microbial felons may have an advantage due to their possessing specialized ways to attach to the blood type antigens in the gut, which makes infection much easier. Many of these 'molecular suction cups' are adhesive-type lectins, a class of proteins also found in many foods. A huge amount of research has been done correlating the differences in resistance to pathogenic microorganisms that exist between the different blood types. Historically, some of the most catastrophic epidemic and endemic diseases are ABO selective, and in many instances demonstrate ABO related differences in morbidity (sickness), mortality (death), or the level of the inflammatory response to the infection. Here are just a few:
This is especially interesting in light of the fact that many of the fucosyltransferase enzymes convey blood group and/or secretor status. (15) Human feces contain enzymes produced by enteric bacteria that degrade the A, B, and H blood group antigens of gut mucin glycoproteins. The autosomal dominant ABH secretor gene together with the ABO blood group gene controls the presence and specificity of A, B, and H blood group antigens in human gut mucin glycoproteins. There is evidence that the host's ABO blood group and secretor status affects the specificity of blood group-degrading enzymes produced by his fecal bacteria in vitro. (16) Comparatively small populations of fecal bacteria produce blood group-degrading enzymes but their presence is highly correlated with the ABO /secretor phenotype of the host: Fecal populations of B-degrading bacteria were stable over time, and their population density averaged 50,000-fold greater in blood group B secretors than in other subjects. In fact, the large populations of fecal anaerobes may be an additional source of blood group antigen substrate for blood group antigen degrading bacteria: antigens crossreacting with blood group antigens were detected on cell walls of anaerobic bacteria from three of 10 cultures inoculated. (17) Gut bacteria can have direct effects on gene activation that may be essential for proper gut development. Bacteria induced expression of mammalian genes has been known since the 1980's when Japanese researchers were able to show that a fucosyltransferase enzyme (fucosyl-asialo GM1) was induced by bacteria but was absent from germ-free strains. (14) This is especially interesting in light of the fact that many of the fucosyltransferase enzymes convey blood group and/or secretor status. (15) ABO blood groups and infectious disease The previous section appears to imply a selection disadvantage for group A, and it has been argued that under present day civilized living conditions O carriers have a preservation advantage over blood group A. (52) This may be the result of the deletion of the selection factor “infectious disease” which may nevertheless regain importance if environmental changes occur. (53) Infectious diseases, especially the worldwide epidemic diseases, have to great extent selective effects. This is demonstrated inter alia in the different "selection values" in the ABO blood group system. During the eons prior to anti-microbial intervention, selection variability via ABO polymorphism was the preeminent natural survival mechanism. A morbidity and mortality variation among the ABO and secretor groups is presented in the following tables. A special examination of polymorphic differences in uropathic infectious disease is presented in the final table. For a more detailed examination of particular infectious scenarios, the reader is referred to a previous comprehensive survey by the author. (54) Class Mechanism Description Example Selectivity Adhesion kinetics Adhesin or lectin specificities of the infectious agent based on particular ABH glycosylation • Candida albicans (group O) Humoral dynamics Inadequate isoagglutinin production or activity • Neisseria gonorrhoeae (group B) Molecular mimicry Infectious agent is antigenically similar to host's ABO group • Giardia lamblia (group A) Response variability Host response Variation in severity of disease through unique biologic response (examples: inappropriate inflammatory response; rosette formation) • Cholera (group O) • Dengue Fever (group B) • Malaria (group A) Substrain susceptibility Different ABO groups often show variations in susceptibility between individual bacterial, fungal, or parasitic species or viral strains. • Influenza (all groups) • Malaria (group O versus group A) Figure 6.3.6 Mechanisms of ABO influence on infectious pathology This includes cholera (O), smallpox (A), malaria (A) and influenza (variable subsets depending on strain). The influence of ABO polymorphism on infectious disease appears to stem from a multitude of unique factors. They are summarized on the following pages. 50.34% of patients were ABH antigen secretors and 45.51% non-secretors. Distribution analysis of blood group revealed that 40 blood group B, 67 blood group A 20 blood group O and 19 blood group AB patients secreted ABH antigens in saliva. Fifty-six blood group O, 19 blood group B, 32 blood group A and 17 blood group AB patients were non-secretors. Gastroduodenal complaints were common among non-secretors. Sixty-two percent of patients with a combination of duodenal ulcer and gastro-oesophageal reflux and 54% of patients with gastritis were non-secretors. Of 290 samples, 31.02% were positive for H. pylori. Thirty percent of these tested positive for babA gene; the majority belonged to non-secretor blood group O. CONCLUSIONS: Our results suggest that the infection of H. pylori is correlated with ABO blood groups and blood group antigens secretion in body fluids. https://www.ncbi.nlm.nih.gov/pubmed/25322664 Strain Susceptible phenotype Comments Amoebic dysentery O, A • Blood groups B and AB have a degree of resistance against developing severe or acute dysentery, especially the amoebic forms Candida carriage O, NS • Candida carriage was associated with blood group O (P < 0.001) and, independently, with non-secretion of blood group antigens (P < 0.01) • Candida albicans extracellular polymeric material (EP) contains a mannoprotein adhesin with a lectin-like affinity for H (type 2) blood group antigen • There were a significantly higher number of non-secretors (48.9%) among 174 patients with either oral or vaginal candida infections compared with the proportion of non-secretors in the local population (26.6%). Non-secretor saliva actually seemed to enhance Candida attachment Cholera O, AB • Blood group O individuals have a greater risk of infection with cholera and develop the most severe and life threatening forms of this illness. This has been documented in several studies • Type AB's on the other hand appear to have the highest degree of protection from cholera infections • Type O had more diarrhea-like stools per day than persons of other blood groups, were more likely to report vomiting and muscle cramps Coccidioidomycosis B • Blood group B individuals are more prone to disseminated disease following exposure. Dengue Fever B • According to researchers, blood group B was strongly associated with the severe form of dengue fever known as dengue hemorrhagic fever. Dermatophytosis A • The fungus Trichophyton rubrum, isolated from 54.5% of the patients tested, was more frequent in individuals belonging to blood group A E. Coli Variable subsets • It appears that many forms of E. coli capable of causing diarrhea are immunologically “B-like.” This results in a substantially higher number of cases of diarrhea among individuals of blood group B and AB people • However, when it comes to the overall severity of infection with E. coli, type B and AB are not alone; type O's also are more likely to get a severe form of diarrhea Figure 6.3.7 Influence on ABO polymorphism on susceptibility to various infectious agents. From: D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev 2001; 6(4):390-405 Strain Susceptible phenotype Comments Giardia A • Blood group A is more susceptible to giardiasis especially the asymptomatic form, while blood group B was less susceptible to giardiasis. Helicobacter pylori O, non-secretor • H. Pylori variants produce a variety of blood group antigens, including A, Lewis (a) and a variety of type 1 H like antigens (O) • Group O would be a moderate risk factor for infection by Helicobacter pylori, with more severe cases in men. • Group O has a more pronounced inflammatory reaction to H. pylori. Group O cells released significantly more IL-6 and TNF in response to H. pylori infection. • The Lewis (a + b-) non-secretor phenotype and blood group O are relevant genetic markers of peptic ulcer. • The Lewis (a+ b-) non secretor phenotype and blood group A were all positively associated with esophageal adenocarcinoma, with concurrent H. pylori infection Hookworm O • A 1972 Egyptian study correlated type O with higher incidence of hookworm and strongyloidiasis. Influenza Variable subsets • Blood group A: Generate a quick and substantial antibody response against influenza type A (H1N1) and especially A (H3N2). The antibody response against influenza B is not quite as dramatic. • Blood group AB: Relatively poor ability to generate high antibody levels against any of the influenza viruses. • Blood group B: Reasonable, but not great ability to generate an antibody response against influenza A (H1N1). Slowest (3-5 months) and weakest ability to generate antibodies against influenza A (H3N2 “Hong Kong”) of any blood group. Against influenza B virus, blood group B has a significant advantage and responds differently from either blood group A or O. The blood group B immune response happens much earlier and persists longer. • Blood group O: Moderate ability to generate antibody response against influenza A (H1N1) and A (H3N2) viruses. Antibody response against influenza B is not as dramatic as blood group B. Malaria A, AB • The evidence suggests that blood group A individuals might have a higher predisposition to infection with the Plasmodium vivax species while blood group B individuals tend toward higher infection rates with P. falciparum. • Malaria infected red blood cells sometimes bind to uninfected red blood cells to form clumps, called rosettes. The rosettes can obstruct flow in small blood vessels and lead to tissue damage and severe malaria disease. The tendency for malaria to be worse among A's and AB's is due primarily to a greater degree of rosette formation by RBC's with these antigens. • Von Willebrand Factor, always elevated type A, also enhances rosette formation Figure 6.3.7 (continued) Influence on ABO polymorphism on susceptibility to various infectious agents. From: D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev 2001; 6(4):390-405 Strain Susceptible phenotype Comments Neisseria gonorrhoeae B • The relation of infection with Neisseria gonorrhoeae to the blood groups A, B, AB, and O was examined in 584 women attending a prenatal clinic. The occurrence of gonorrhea was significantly higher in black patients with blood group B than in those with blood groups A, AB, or O. Depending on the ABO blood group, gonorrhea may affect the titers of isohemagglutinins compared with those of uninfected controls. • The isohemagglutinin titers in group O patients were significantly increased (P less than 0.001) against erythrocytes A, B, and AB. In group A patients, only the titer against AB erythrocytes was significantly increased. • In group B patients, the titer against AB erythrocytes was significantly lower (P less than 0.001) as compared with that in sera of healthy persons. Norwalk Virus (Norovirus) O • It appears that group O RBC's are most easily bound by Noroviruses (NV) versus group B RBC's that are apparently little bound, if at all. Individuals with an O phenotype were more likely to be infected with NV. • The preferred binding sites are apparently the H type 2 antigen that functions as the viral receptor on human type O RBC's. • The Lewis B antigen (found in secretors) is also a binding site. Schistosomiasis A • Group A tends to be more susceptible to infection, tends to get more intense symptoms following infection, and is much more likely to have damage to organs (like the liver) following infection. Shigellosis B, AB • A strong association between blood group B (and AB to a slightly lesser degree) and shigellosis exists. Smallpox A • Group A has higher mortality from smallpox infection • Group A individuals also have more reactions from smallpox vaccination. • The leukocytes of peripheral blood of group A individuals showed a poorer binding capacity with respect to the smallpox vaccine virus. • Blood group A also exhibited a high rate of chromosomal aberration after vaccination, resulting to some extent from increased proliferative ability of the cells. Staphylococcus aureus A • Blood group A is much more likely to be a chronic carrier of Staphylococcus aureus. This is partly due to blood group A individuals having a decreased ability to mount an aggressive antibody (or immune) response against this organism. Streptococcus (Group B) B • A blood group connection with neonatal group B streptococci infection exists for blood group B. Maternal blood group B associated with about a doubling of risk for infection among their infants. Strongyloidiasis O • A 1972 Egyptian study correlated type O with higher incidence of hookworm and strongyloidiasis. Tuberculosis O • Group O blood has a much higher rate of infection with tuberculosis (this is particularly true in individuals of European descent). • Tuberculosis runs a much more aggressive and detrimental course in blood group O, while type A are afforded the highest degree of protection. • Typically, during the first two years of infection with bacillary tuberculosis, there is a significant excess of infection among individuals with blood group O and AB. Figure 6.3.7 (continued) Influence on ABO polymorphism on susceptibility to various infectious agents. From: D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev 2001; 6(4):390-405 Blood group Uropathogenic Strains A • Staphylococcus saprophyticus B • Klebsiella pneumoniae • Proteus spp. • Pseudomonas sp. AB • Klebsiella pneumoniae • Proteus spp. • Pseudomonas spp. • Staphylococcus saprophyticus Non-secretor • Uropathogenic E. coli As a rule, blood group B is most plagued by chronic or recurrent UTI's. Type AB is next on the susceptibility list, followed by type A Type O's are the most protected. Non-secretors are much more prone to repeated and severe UTI's. Figure 6.3.8 Influence on ABO polymorphism on susceptibility to various uropathic infectious agents. From: D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev 2001; 6(4):390-405 Secretor status and Candida carriage ABH non-secretors are much more likely to be carriers of Candida sp. and to have problems with persistent Candida infections. Blood group O non-secretors are the most affected of the non-secretor blood types. One of the innate defenses against superficial infections by Candida species appears to be the ability of an individual to secrete the water-soluble form of his ABO blood group antigens into body fluids. The protective effect afforded by the secretor gene might be due to the ability of glycocompounds in the body fluids of secretors to inhibit adhesins (attachment lectins) on the surface of the yeast. In attachment studies, preincubation of blastospores with boiled secretor saliva significantly reduced their ability to bind to epithelial cells. ABH non-secretor saliva did not reduce the binding and often enhanced the numbers of attached yeasts. (163,164) In one study, among individuals with Type II diabetes, 44% of ABH non-secretors were oral carriers of this yeast. (165) Although non-secretors make up only about 26% of the population, they are significantly over represented among individuals with either oral or vaginal Candida infections, making up almost 50% of affected individuals. (168) The inability to secrete blood group antigens in saliva also appears to be a risk factor in the development or persistence of chronic hyperplastic candidosis. In one study, the proportion of non-secretors of blood group antigens among patients with chronic hyperplastic candidosis was 68%. (166) Women with recurrent idiopathic vulvovaginal candidosis are much more likely to be ABH non-secretors. Combining both ABH non-secretor phenotype and absence of the Lewis gene, Lewis (a- b-), the relative risk of chronic recurring vulvovaginal candidosis is between 2.41-4.39, depending on the analysis technique and control group. (167) Oral carriage of Candida is also significantly associated with blood group O (p < 0.001) and independently, with non-secretion of blood group antigens (p < 0.001), with the trend towards carriage being greatest in group O non-secretors. (168) Secretor status influence on breast milk composition Human breast milk is the most heavily fucosylated of all the higher mammals. Specific human milk oligosaccharides, especially fucosylated neutral oligosaccharides, protect infants against specific microbial pathogens. The oligosaccharide composition of human milk varies considerably from person to person; however, and suggests the existence of many genotype subpopulations. This variation in individual oligosaccharide concentrations suggests that the protective activities of human milk could also vary among individuals and during lactation. (32) Fucosylation profiles of human milk oligosaccharides are known to vary by host ABO and Lewis blood groups and ABH secretor status via the FUT2, FUT3, and FUT4 family of fucosyltransferases. (33,34) During the first week of lactation, the ability to produce neuraminyloligosaccharides is linked to the ABH secretor groups. Moreover, the ability to produce oligosaccharides with Le (a) or Le (b) characteristics is linked to Lewis and Secretor systems. The consequences of this are that secretors will produce higher levels of N-acetylneuraminic acid and lower levels of galactose in their breast milk than non-secretors. In the ABH secretor groups, blood group A and O secretors also have higher N-acetylglucosamine contents than B and AB secretors (p less than 0.001), while the A and B secretors have higher galactose levels. A significantly higher level of fucose also distinguishes the Lewis secretor groups. The ABH (+), Le (a-b-) group had higher lactose contents than the other groups. (35) Maternal ABO Blood Group, ABH secretor status and Lewis Phenotype Composition of Breast Milk A or O, Secretors, Lewis (a-b+) • High amounts of n-acetylneuraminic acid and n-acetylglucosamine • Lower levels of galactose • Higher fucose • Lower lactose • Presence of Le(b) and either A or O substances B or AB, Secretors, Lewis (a-b+) • High amounts of n-acetylneuraminic acid • Lower n-acetylglucosamine • Moderate galactose • Higher fucose • Lower lactose • Presence of Le(b) and either B or AB substances ABO non-secretors, Lewis (a+b-) • Highest galactose • Lowest amounts of N-acetylneuraminic acid • Higher fucose • Lower lactose • Presence of Le(a) and absence of ABO substances ABO, Lewis negative, Lewis (a-b-) • No Lewis substances • Highest lactose • Quantities of ABO substances, galactose, n-acetylneuraminic acid and n-acetylglucosamine cannot be estimated Figure 6.3.5 Differences in carbohydrate composition of human milk oligosaccharides by ABO and Lewis blood groups and ABH secretor status. (From D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev. Aug; 6(4):390-405; 2001) The neuroplasticity that characterizes human adaptive learning may have a sweet tooth for fucose. Fucose is now garnering attention as an important component in learning: brain fucosylation skyrockets during periods of intense learning, which appear to correlate with increased ligand-like activity involving fucose at the neurosynaptic juncture. Inhibition of protein fucosylation using 2-deoxy-D-galactose causes amnesia in animals, presumably by blocking formation of fucose α(1-2) galactose linkages, whereas administration of free L-fucose in rats enhances memory retention and long-term potentiation (LTP), a widely accepted cellular model for memory. (36) It appears that what goes into holding the synapse together may be as important a factor in cognition and learning as what jumps across the synapse. 15. D'Adamo PJ, Kelly GS. Metabolic and immunologic consequences of ABH secretor and Lewis subtype status. Altern Med Rev. Aug;6(4):390-405; 2001 This is especially interesting in light of the fact that many of the fucosyltransferase enzymes convey blood group and/or secretor status. (15) 16. Hoskins LC, Boulding ET. Degradation of blood group antigens in human colon ecosystems. I. In vitro production of ABH blood group-degrading enzymes by enteric bacteria. J Clin Invest Jan;57(1):63-73;1976 17. Hoskins LC, Boulding ET. Degradation of blood group antigens in human colon ecosystems. II. A gene interaction in man that affects the fecal population density of certain enteric bacteria. J Clin Invest Jan;57(1):74-82; 1976 14. Umesaki Y. Immunohistochemical and biochemical demonstration of the change in glycolipid composition of the intestinal epithelial cell surface in mice in relation to epithelial cell differentiation and bacterial association. J Histochem Cytochem. 1984 Mar; 32(3):299-304. 163. Toft AD, Blackwell CC, Saadi AT, et al. Secretor status and infection in patients with Graves” disease. Autoimmunity 1990; 7(4):279-89. 164. Blackwell CC, Aly FZ, James VS, et al. Blood group, secretor status and oral carriage of yeasts among patients with diabetes mellitus. Diabetes Res 1989 Nov; 12(3):101-4. 165. Thom SM, Blackwell CC, MacCallum CJ, et al. Non-secretion of blood group antigens and susceptibility to infection by Candida species. FEMS Microbiol Immunol 1989 Jun; 1(6-7):401-5. 166. Lamey PJ, Darwazeh AM, Muirhead J, et al. Chronic hyperplastic candidosis and secretor status. J Oral Pathol Med 1991 Feb; 20(2):64-7. 167. Chaim W, Foxman B, Sobel JD. Association of recurrent vaginal candidiasis and secretory ABO and Lewis phenotype. J Infect Dis 1997 Sep; 176(3):828-30. 168. Burford-Mason AP, Weber JC, Willoughby JM. Oral carriage of Candida albicans, ABO blood group and secretor status in healthy subjects. J Med Vet Mycol 1988 Feb; 26(1):49-56. 169. 168 Thom SM, Blackwell CC, MacCallum CJ, et al. Non-secretion of blood group antigens and susceptibility to infection by Candida species. FEMS Microbiol Immunol 1989 Jun; 1(6-7):401-5. The Gut Microbiota for Health meeting (Barcelona, Spain, March 13-15) particularly emphasized the applications of gut microbiota science. Scientists haven't yet identified the 'healthiest' microbial composition, but what's clear so far is that a diverse colonizing microbiota is important: more diversity means greater resilience, with the potential to make you generally healthier and able to resist specific diseases. With input from other GMFH board members, I have created a list of practical recommendations which, to the best of our current knowledge, increase the diversity of microbes colonizing your gut: Eat a diverse diet Consume fermented foods with live microbes; they have at least a transient effect Eat washed raw fruits and vegetables, which harbor environmental microbes (not recommended if you have difficulties digesting raw vegetables) Consider consuming probiotic-containing foods/supplements; look up the controlled trials for evidence of health benefits from specific probiotics Consume adequate levels of diverse types of fiber, including prebiotics, to promote a diverse microbiota; this might mean consuming 2-3 kinds of fruits or vegetables in one sitting Breast feed your baby; breast milk contains live microbes and a rich supply of oligosaccharides that appear to enrich good bacteria in the baby's gut Avoid elective caesarean births; if one is medically necessary, talk to your pediatrician about swabbing the newborn with mom's vaginal flora, as in a procedure being investigated by Maria Gloria Dominguez Bello Avoid unnecessary antibiotics Wash hands with soap and water instead of sanitizing Live on a farm, or at least have a dog or two; this seems especially beneficial for children if started when they are babies And if you want to know more about the world inside you, check out these non-profit projects, which allow you to get your microbiota assayed and compare your microbial diversity to others in the project: Reviewed and revised on: April 4, 2015

|
The statements made on our websites have not been evaluated by the FDA (U.S. Food & Drug Administration).
Our products and services are not intended to diagnose, cure or prevent any disease. If a condition persists, please contact your physician.
Copyright © 2015-2023, Hoop-A-Joop, LLC, Inc. All Rights Reserved. Log In



